Table of Contents
ToggleAt MSI we often get asked the question, “How old do you have to be to get a vasectomy?” Well, legally anyone over the age of 18 is allowed to have one, but the age of men who have vasectomies can vary as much as their reasons for getting one.
Unfortunately at MSI Australia, we cannot offer vasectomy on men with no biological children under 25 because none of our doctors are prepared to do this because of the high risk of regret and wanting to reverse the operation in this group of men.

Who is the right candidate for a vasectomy?
Vasectomy is a method of contraception for people who have decided that they don’t ever want children, or who have children and are certain they don’t want more. Both of these decisions require a level of emotional and intellectual maturity because they will have permanent consequences.
Men under the age of 25, who have not had biological children, may not have had the opportunity to thoroughly consider the impact of this decision on their life, or on the life of their current or future partner. For this reason, our vasectomy doctors are uncomfortable performing permanent sterilisation on men under 25 years old.
So are most men between 25 and 30 excluded?
No, this does not mean that men between 25 and 30 are excluded from being able to have the procedure, but that doing so will require a consultation with a counsellor and the vasectomist around the reasons they are electing to have the procedure done.
For instance, some young men will choose to have a vasectomy in order not to pass on any serious health concerns they know to be genetic. In this case, their age may not be an excluding factor.

Reasons for choosing a vasectomy
Men opt for a vasectomy for various reasons, such as having completed their family or desiring permanent birth control. While it can be done at a relatively young age, most doctors recommend considering vasectomy reversals and other temporary birth control methods before making a decision.
Before having a vasectomy
Before having your vasectomy, there are a few factors that you should consider:
Research your options
Before deciding on a vasectomy, explore alternative birth control methods and discuss your decision with your partner. Understand the pros, cons, and limitations, including the fact that vasectomy does not protect against sexually transmitted infections.
Choose the right healthcare provider
Select a healthcare provider experienced in vasectomies, and consider factors such as their success rate, experience and patient reviews. Discuss any concerns, including the recovery process and when to resume sexual activity.
Ask questions during your consultation
During your consultation, inquire about the vasectomy procedure, potential complications, and the recovery process. Make sure you ask questions such as ‘When it’s safe to resume sexual intercourse?’ and any necessary precautions.
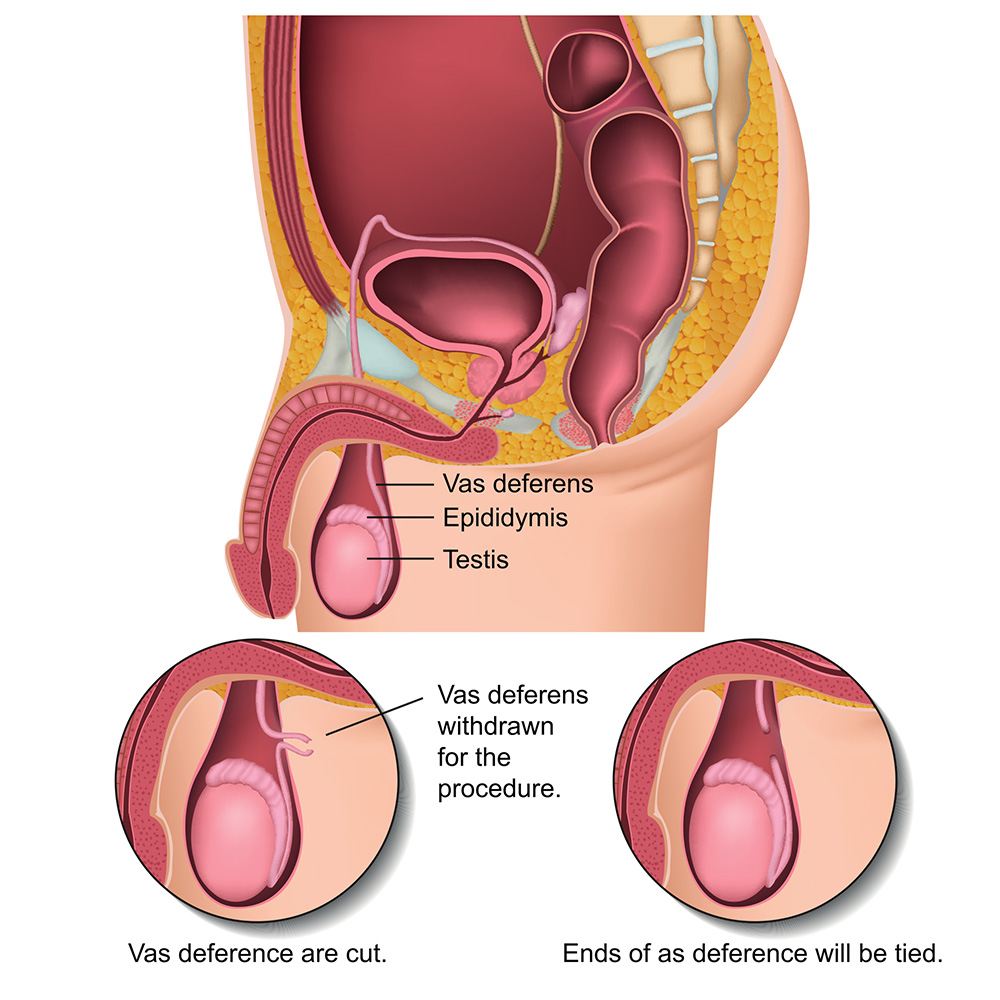
What to expect during the procedure
During the vasectomy procedure, the doctor will numb the area with a local anaesthetic. They will then either make a small puncture in the scrotum to access the vas deferens. The tubes are then cut to prevent sperm from entering the semen.
Recovery process
After a vasectomy, patients typically experience mild discomfort and swelling. Most men can return to work within a few days and resume sexual activity within a week. Complications are rare but may include infection, haematoma or very rarely a failure of the operation requiring a redo operation.
Reversing a vasectomy: is it possible?
While vasectomies are considered a permanent form of birth control, it is possible to reverse the procedure in some cases. However, even with a successful reversal, there is no guarantee of achieving pregnancy, and couples may need to explore alternative fertility options.
Vasectomy Reversal: How it works
Vasectomy reversal is a surgical procedure that reconnects the vas deferens, allowing sperm to be present in the semen again. While it’s possible to reverse a vasectomy, success rates vary depending on factors such as the time since the original procedure and the surgeon’s expertise.
Success rates and factors affecting reversal
Vasectomy reversal success rates range from 40-90%, depending on factors like the surgeon’s skill, the time elapsed since the vasectomy, and the patient’s overall health. However, a successful reversal does not guarantee pregnancy, as other factors may also impact fertility.
Alternatives to vasectomy reversal
For those seeking alternatives to vasectomy reversal, options such as in-vitro fertilisation (IVF) or intra-cytoplasmic sperm injection (ICSI) can help achieve pregnancy. These procedures involve extracting sperm directly from the testicles and combining it with an egg in a lab setting.
Summary
When deciding on whether to have a vasectomy in Sydney, it is less an issue of age and more a case of ensuring you have thoroughly assessed your feelings on the matter and are choosing to do so for the right reasons.
Can you be too old to have a vasectomy?
There is no age limit for getting a vasectomy, as long as you are healthy enough to undergo the procedure. However, if you are considering a vasectomy later in life, it is important to understand that the procedure is permanent and should only be done if you are sure that you do not want to father children in the future.
How effective is a vasectomy?
Vasectomy is a highly effective form of birth control, with a failure rate of approximately 0.1%. However, it is important to remember that vasectomy does not provide protection against sexually transmitted infections, so it is still important to use condoms or other forms of protection.
Is a vasectomy similar to female tubal ligation?
While both vasectomy and tubal ligation are permanent methods of birth control, they are different procedures. However, a vasectomy is a simpler procedure and less expensive than tubal ligation.
Will it affect my sexual function/ability to ejaculate?
No, a vasectomy does not affect sexual function or the ability to ejaculate. The procedure simply blocks the vas deferens, preventing sperm from entering the semen. This means that while sperm is no longer present, the volume, appearance, and sensation of the ejaculate remain largely unchanged. Men can continue to enjoy sexual intercourse and achieve orgasms as before, without any noticeable difference in their sexual experience.
Will a vasectomy affect my testosterone levels?
Vasectomy should not affect your testosterone levels, as the procedure does not involve the testicles, where testosterone is produced. There is no evidence to suggest that vasectomy has any effect on hormone levels or sexual function.