Table of Contents
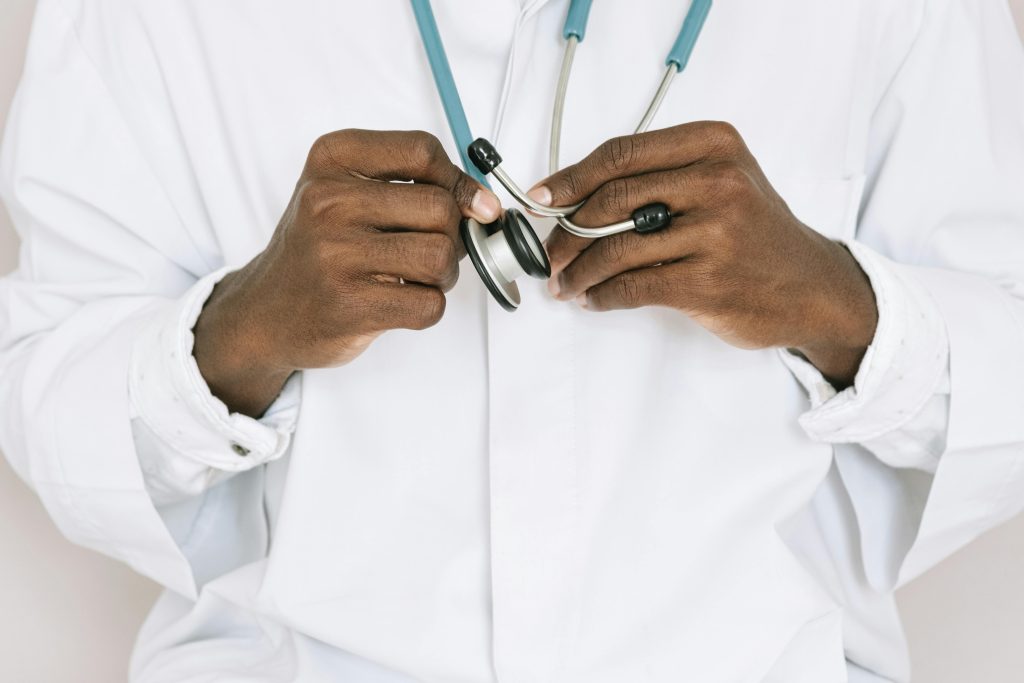
ToggleIf you’re in a heterosexual, monogamous relationship and have decided not to have any/more children, then you and your partner might be weighing up your options around permanent contraception methods, also referred to as sterilisation. The two to consider are tubal ligation and vasectomy.
Tubal ligation
Tubal ligation involves making an incision in the abdominal wall, locating the fallopian tubes and closing them.
There are many methods of closing the fallopian tubes: they can be cut and then tied off, clamped or cauterized. Alternatively, they might be kept whole but closed with a clip, band or ring.
Tubal ligation is a more complex procedure than a vasectomy and involves going under general anaesthetic and several scalpel incisions.
After the procedure, most women will spend several hours in the hospital, however, since it’s often performed as part of another procedure, (such as a c-section) they may stay longer.
Post-procedure, patients can expect symptoms such as shoulder pain, sore throat, bloating, and vaginal bleeding and discharge. These will last around two to four days, and most patients can resume their normal routine after this. However physical activities should be avoided for the first week after surgery, and anything involving heavy lifting should be avoided for around three weeks.
Tubal occlusion
Tubal occlusion involves inserting a small coil into the fallopian tube via a catheter through the vagina. The coil then induces the body to form a barrier around it, much like scar tissue, that then creates a natural blockage in the fallopian tube.
Tubal occlusion is not currently available in Australia due to the product being recalled by the manufacturer after the Therapeutic Goods Administration issued a hazard alert.
Vasectomy
There are two types of vasectomy: closed and open-ended. In a closed-ended vasectomy, the two ends of the vas deferens are sealed. In an open-ended vasectomy, the end connected to the testicles is left open, which allows the sperm to freely escape into the intra-scrotal space. The sperm then die and are reabsorbed by the body. The end connected to the prostate gland is closed permanently which leads to sterility. Both are equally effective, however an open-ended is considered the best option as it has far fewer complications.
A vasectomy is performed under local anaesthetic, with patients having the option to choose twilight sedation if desired. The whole process takes around 15 minutes and patients can leave almost immediately after the procedure, which is available in Canberra.
Post-procedure patients can expect minor discomfort for 2-3 days and occasionally some mild swelling or bruising which can be treated with Paracetamol and a properly applied ice pack.
Strenuous physical activity and non-contact sports should be avoided for two weeks, and contact sports should be avoided for one month.
Weighing up your options
Efficacy
There is no real difference in the efficacy rate between the two procedures; both have a higher than 99% success rate. However, experienced vasectomy surgeons typically have success rates greater than 99.9% equivalent to failure rates of less than 1 in 1000.
After tubal ligation, the patient is considered sterile and there are no follow-up tests. After vasectomy, the patient needs to use birth control for an additional three months until they’ve had a semen test to confirm the success of the operation.
Cost
Vasectomy is the more affordable procedure. With private health insurance, you can be completely covered with no gap or a minimal fee under $100. Tubal ligation, because it involves a general anaesthetic, is more expensive and often costs around $4500.
Safety
Both procedures are incredibly safe, however, because the tubal ligation involves a general anaesthetic and scalpel incisions, it is subject to the usual risks associated with this, such as nausea, vomiting, infections, bruising, bleeding and issues with bladder or bowel function. These complications are rare though.
In addition, tubal ligation has a greater risk of ectopic pregnancies occurring. Around 1 in 200 women may still fall pregnant due to an incomplete closure of the fallopian tubes, if this happens the pregnancy may develop outside the uterus (ectopic pregnancy). This can be a painful and dangerous condition that requires emergency surgery.
By contrast, vasectomy patients are not subject to either a scalpel or general anaesthetic so the largest risks they face are bruising, infection and swelling. Some experience epididymitis, which can be resolved with antibiotics. A small percentage of patients might experience a hematoma, where a blood vessel forms a clot; however, this is typically reabsorbed by the body.
Reversal
Both procedures should be considered permanent. These are not procedures you should undergo if you are unsure about whether you would still like to have children. Even though both tubal ligation and vasectomy are technically reversible, the success rates will depend largely upon how long ago you had the procedure done. Reversals are expensive and usually not covered by insurance. We do not perform reversals.
Last thoughts
Ultimately, this comes down to lifestyle and personal choice. A vasectomy is preferable for most couples, including those in MSI Australia, as it has lower rates of complications, is a simpler procedure and costs less. However, tubal ligation is still a very reliable and safe method of sterilisation that many women might choose to undergo for peace of mind.